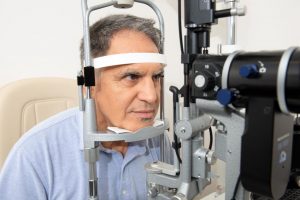
Lately new technologies support dry eye centers in the evaluation of the type of Dry Eye Disease and thus in the choice of the appropriate and tailored treatments.
First of all the diagnosis classifies dry eye into the two major subgroups Evaporative Dry Eye Disease and Aqueous deficient.
Like every medical condition your doctor will start the diagnosis with a comprehensive medical interrogation and the use of questionnaires including symptoms description, medical history, systemic diseases and routinely used drugs. Typical questionnaires for dry eye are presented below for your information: OSDI, IDEEL and SPEED, Attached below the OSDI questionnaire for your impression:
In the next phase, your doctor will be examining you. The clinical tests divides into classical approach and advanced.
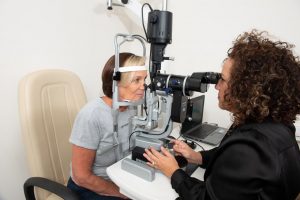
Classic approach
an ophthalmic clinical exam always includes slit lamp examination (the machine in which you put your forehead and chin and the doctor looks at your eye with a white or blue light). This machine allows your eye doctor to look at the various parts of your eyes: the conjunctiva, cornea, eyelids etc.
Apart from looking at all the structures of your eye, your ophthalmologist may perform the following test at the slit lamp:
Shirmer test – The Shirmer test measures the secretions of the lacrimal gland. A calibrated filter paper strips are placed in the temporal third of the lower eyelid and, with your eyes closed, wetting of the strip is measured after 5 minutes.
In aqueous-deficient dry eye values are reduced, a Shirmer test of less than 5mm is pathological and may indicates Sjögren’s syndrome.
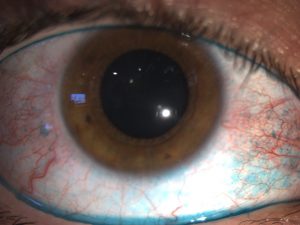
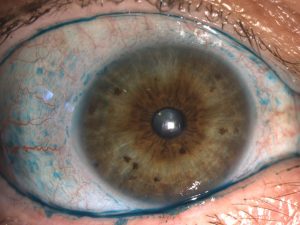
Staining – Topical dyes reveal certain features of the ocular surface, fluorescein, rose bengal and lissamine green are available to diagnose dry eye. Fluorescein is a stain that marks the tear film and defects in the corneal, as well as determines the tear break-up time. By observing with cobalt blue light of a slit lamp the time between the last blink and the appearance of the first dry spot or hole in the tear film is measured. The Tear break up time describes the stability of the tear film: the time required for the ocular surface to lose cohesive surface wetting after each blink. When TBUT is less than the blink rate, the cornea is left unprotected, and thus dries and the signs and symptoms of dry eye are exacerbated.
Rose bengal and lissamine green highlights superficial damaged cells, revealing the areas of your conjunctiva and cornea that are not hydrated and protected as they should be if there is no dry eye. This Topical stains are useful to grade the severity of your dry eye disease.
Advanced
In the last years, with the widespread of dry eye syndrome related to the modern life, new technologies have been developed to help understand and diagnose the exact cause and the severity of your disease. They rely on biological analysis of the tears and various Imaging technologies of the lacrimal system.
Osmolarity – In the same way that blood test allow us to diagnose diabetes or other chemical pathologies, it is possible to evaluate the function of the tear system by analyzing the composition of your tears. At the dry eye center a very small sample of your tears (50nL) is collected in non-invasive way from the corner of your eyelid. A Pipette is applied to the corner of your eyes in a not painful manner. The pipette is then placed in a mini laboratory that will give an immediate result upon examination.The tears osmolarity is the concentration of minerals like Sodium (salt) in your tears. It is measured by using Tearlab osmolarity system, Abnormal osmolarity is defined by one of the two:
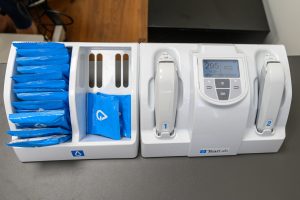
- An elevated reading above 300mOsm/L (which is similar to our body osmolarity), indicating that your tears are more concentrated thus the burning and itching sensation.
- An Inter- eye difference above 8mOsm/L indicates that the tear system is challenged and works in an irregular manner.
Abnormal osmolarity is the hallmark characteristic of dry eye syndrome. It is the most sensitive and reliable measurement of Dry Eye, it is useful for diagnosis as well as follow- up of the disease.
Interferometry – imaging the surface contour of the tear film and analyzing the thickness of the lipid layer is called Lipid layer interferometry. A specific type of camera records the way that the lipid layer spreads and evaporates on the cornea. It measures tear stability and the quality of the oils that your Meibomian Glands produce.
Thinning of the tear film lipid layer will show up into discontinuous patchy regions of cornea with no protection of the oils, denoting an unstable tear film. When the interferometry shows a thinning of the lipid layer it indicates Meibomian gland dysfunction. Interferometry is very useful in diagnosing the presence and the severity of your dry eye.
Meibography – is a recently developed technology. It measures the number and the quality of your meibomian glands which as we explained earlier are producing the critical lipid layer of your tears. It is non-invasive and relies on Infrared technology. The high definition images of the Meibomian provides information on tissue damage, meaning the severity of the disease. It is also a great tool for measuring the effectiveness of the treatments.